Struggling to conceive? Intracytoplasmic Sperm Injection (ICSI) could be the game-changer you’re looking for. As a specialized form of in vitro fertilization (IVF), ICSI helps couples overcome male infertility and other conception hurdles by directly injecting a single sperm into an egg. In this 2025 guide, we’ll break down how ICSI works, its success rates, costs, and whether it’s right for you. Let’s dive into the world of assisted reproductive technology (ART) and explore why ICSI is a beacon of hope for many.
What Is ICSI and How Does It Fit Into IVF?
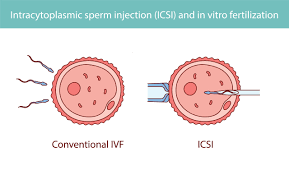
ICSI, or Intracytoplasmic Sperm Injection, is a cutting-edge fertility treatment designed to tackle severe male infertility issues, such as low sperm count or poor sperm motility. Unlike traditional IVF, where sperm and eggs mingle in a lab dish, ICSI takes a more hands-on approach. A skilled embryologist selects a healthy sperm and injects it directly into a mature egg using a tiny microneedle, ensuring fertilization happens. This makes ICSI a go-to solution for couples facing challenges that standard IVF can’t address.
Step-by-Step: How the ICSI Process Works
Curious about what happens during ICSI? Here’s a clear, step-by-step look at the procedure:
-
Ovarian Stimulation: Medications encourage the ovaries to produce multiple eggs, tracked through ultrasounds and blood tests.
-
Egg Retrieval: A minor procedure collects mature eggs from the ovaries under sedation.
-
Sperm Collection: Sperm is gathered, either through ejaculation or surgical methods like testicular sperm extraction for cases like azoospermia.
-
Sperm Injection: Using advanced microscopy, a single sperm is injected into an egg to spark fertilization.
-
Embryo Development: Fertilized eggs grow into embryos in a lab for 3–5 days.
-
Embryo Transfer: One or more healthy embryos are placed in the uterus, with extras often frozen for future cycles (frozen embryo transfer, FET).
-
Pregnancy Confirmation: A blood test 10–14 days later checks for a clinical pregnancy.
This precise process maximizes the chances of successful egg fertilization, especially when sperm quality is a concern.
ICSI vs. IVF: What’s the Difference?
Wondering how ICSI stacks up against standard IVF? Here’s the breakdown:
-
IVF: Sperm and eggs are combined in a lab, relying on sperm to naturally penetrate the egg. It’s ideal for couples with healthy sperm parameters.
-
ICSI: A single sperm is manually injected into an egg, perfect for male infertility issues like low sperm count, poor motility, or abnormal sperm shape.
When Should You Choose ICSI?
-
Severe male infertility (e.g., oligospermia or surgically retrieved sperm).
-
Failed IVF cycles due to poor fertilization.
-
Unexplained infertility or poor-quality oocytes.
-
Use of frozen eggs or sperm, where natural fertilization may be less effective.
ICSI’s targeted approach makes it a powerful tool, but it’s not always needed for every IVF case. A fertility specialist can guide you based on your unique situation.
ICSI Success Rates: What to Expect in 2025
ICSI is highly effective at achieving fertilization, with rates of 70–85% per cycle, depending on the clinic. However, the clinical pregnancy rate (successful implantation) typically ranges from 30–45% per cycle, influenced by factors like:
-
Maternal Age: Women under 35 see higher success (40–50% per cycle), while rates drop slightly for older women.
-
Sperm and Egg Quality: Even poor sperm can work with ICSI, but egg quality and chromosomal abnormalities affect outcomes.
-
Clinic Expertise: Top clinics with advanced labs and experienced embryologists boost success.
In 2025, technologies like preimplantation genetic testing (PGT) enhance ICSI outcomes by identifying healthy embryos, making it a promising option for male infertility and beyond.
Risks and Side Effects of ICSI
ICSI is safe but not without risks. Here’s what to consider:
-
Ovarian Hyperstimulation Syndrome (OHSS): A rare side effect from stimulation drugs, causing discomfort.
-
Multiple Births: Transferring multiple embryos increases the chance of twins or triplets.
-
Genetic Risks: A slight risk of chromosomal abnormalities, especially with poor-quality sperm.
-
Birth Defects: Studies suggest a 1–2% higher risk than natural conception, though evidence is mixed.
-
Emotional Toll: The process can be stressful and costly, impacting mental health.
Discuss these with your doctor to ensure ICSI aligns with your goals and health.
Who Is ICSI For? Eligibility and Benefits
ICSI is a lifeline for couples facing specific fertility challenges:
-
Male Infertility: Ideal for low sperm count, poor motility, or abnormal sperm.
-
Failed IVF Attempts: Helps when standard IVF doesn’t result in fertilization.
-
Unexplained Infertility: Addresses hidden barriers to conception.
-
Frozen Gametes: Improves outcomes with frozen eggs or sperm.
-
Older Women: May benefit when egg quality is a factor.
Why ICSI Helps with Unexplained Infertility
For couples with unexplained infertility, ICSI can bypass potential fertilization issues that standard tests miss. By ensuring sperm penetrates the egg, it increases the odds of creating viable embryos, offering hope when answers are unclear.
ICSI Costs in 2025: What You’ll Pay
ICSI costs depend on your location, clinic, and additional procedures. Here’s a 2025 snapshot:
-
United States: $12,000–$15,000 per cycle (plus IVF fees of $10,000–$20,000).
-
India: ₹1,50,000–₹2,50,000 (~$1,800–$3,000).
-
UK: £5,000–£8,000 (~$6,500–$10,500).
-
Australia: AUD 10,000–15,000 (~$6,700–$10,000).
These include medications, lab work, and consultations. Some clinics offer financing or package deals. Contact local providers for accurate quotes.
FAQs: Your ICSI Questions Answered
What’s the difference between ICSI and PICSI?
PICSI selects sperm based on their ability to bind to hyaluronan, potentially improving embryo quality. ICSI uses visual sperm selection.
Is ICSI painful?
Egg retrieval involves mild discomfort under sedation. Sperm collection is usually non-invasive, except in surgical cases.
Does ICSI guarantee a baby?
No, ICSI ensures fertilization but not pregnancy. Success depends on embryo quality, maternal age, and other factors.
How long is an ICSI cycle?
From stimulation to pregnancy test, expect 4–6 weeks per cycle.
Conclusion: Is ICSI Right for You?
ICSI offers hope for couples facing male infertility, unexplained infertility, or IVF challenges. With high fertilization rates and evolving technology in 2025, it’s a powerful tool in the journey to parenthood. Talk to a fertility specialist, explore top clinics, and weigh the costs and benefits to decide if ICSI is your next step. Ready to learn more? Check our resources on fertility treatments or connect with experts today.